Importance
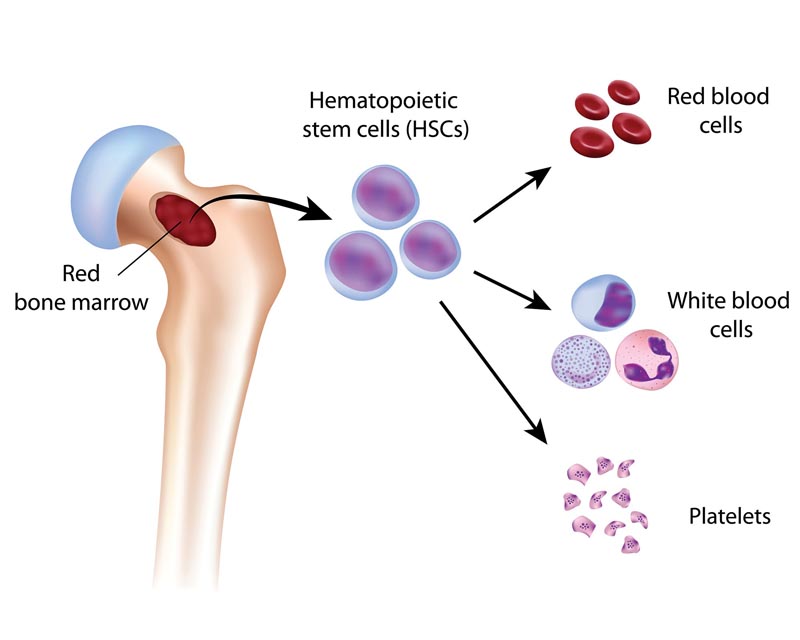
Myelodysplastic neoplasms ( MDS), formerly known as myelodysplastic syndromes, are clonal hematopoietic malignancies that cause morphological dysplasia of the bone marrow along with anemia, neutropenia, or thrombocytopenia.
MDS are associated with an increased risk of acute myeloid leukemia (AML). The annual incidence of MDS is approximately 4 per 100,000 people in the United States and is highest among elderly patients.
Observations
MDS are characterized by a reduced number of peripheral blood cells, an increased risk of transformation to acute myeloid leukemia, and reduced survival. The median age at diagnosis is approximately 70 years and the annual incidence rate increases to 25 per 100,000 in persons aged 65 years or older.
Risk factors associated with MDS include older age and previous exposures to toxins such as chemotherapy or radiation therapy. MDS are more common in men than women (with annual incidence rates of approximately 5.4 vs. 2.9 per 100,000).
MDS typically has an insidious presentation, consisting of signs and symptoms associated with anemia, thrombocytopenia, and neutropenia .
MDS can be classified into subtypes that are associated with a lower or higher risk of AML transformation and that assist with therapy selection. Patients with low-risk MDS have a median survival of approximately 3 to 10 years, while patients with higher-risk disease have a median survival of less than 3 years.
Therapy for low-risk MDS is selected based on whether the primary clinical feature is anemia, thrombocytopenia, or neutropenia . Management focuses on treating symptoms and reducing the number of transfusions required in patients with low-risk disease.
For patients with low-risk MDS, erythropoiesis-stimulating agents, such as recombinant humanized erythropoietin or the longer-acting erythropoietin, darbepoetin alfa, may improve anemia in 15% to 40% of patients for a median from 8 to 23 months. For those with higher risk MDS, hypomethylating agents such as azacitidine, decitabine, or decitabine/cedazuridine are first-line therapy.
Conclusions and relevance
|















