An epidemic of poor psychological health, including high levels of reported depression and anxiety symptoms, accompanied the onset of the COVID-19 pandemic. Adverse mental health is now persistent and widespread in the population; Elevated depressive symptoms continue and are not limited to those who are economically insecure or those most vulnerable to COVID-19 infection and its aftermath.
Despite these strong findings, there is little systematic evidence regarding the specific symptoms of depression and anxiety that are higher during the pandemic and how symptomatology during the pandemic differs from typical patterns.
We assessed the prevalence (proportion of respondents reporting a symptom) and severity (reporting higher intensity of symptoms) of particular symptoms before and during the COVID-19 pandemic. By delving into widely used batteries of screening questions, we identify the key domains that are driving the increase in poor psychological health of the population. This evaluation is imperative for at least two reasons.
First, by investigating specific symptoms , we can distinguish changes in the prevalence from changes in the severity of each symptom. Given the persistence of symptoms throughout the pandemic, the distinction between prevalence and severity is critical in predicting the longer-term consequences of the pandemic both for individual clinical treatment and for resuming work and education as case counts decline. of COVID-19 decrease and lockdown policies.
Second, the study advances knowledge of mental health symptomatology and reporting in the wake of large-scale events such as pandemics and natural disasters. Previous research indicates that event-related mental health problems focus on specific domains rather than the entire depressive syndrome, and these domains vary by context. We contribute to this literature by providing evidence in the context of the COVID-19 pandemic.
The mechanisms underlying the links between the COVID-19 pandemic and psychological distress are unclear. Studies have suggested that uncertainty and social isolation due to lockdowns, as well as complex and changing health guidelines, are likely mechanisms. However, the lack of independent variation in these potential contributing factors complicates the identification of their independent impacts.
Furthermore, psychological distress has persisted beyond the worst of the initial lockdowns. While studies have highlighted the role of infection risk and economic insecurity, little is known about the mental health of populations protected from these direct effects of the pandemic. This study focuses on this population.
Background
The COVID-19 pandemic has been accompanied by substantial increases in adverse mental health, particularly among young people. However, it is unclear to what extent increases in population scores on mental health assessments are due to changes in prevalence, rather than symptom severity.
Furthermore, it is not obvious that widely used assessments of aggregate symptoms retain their typical interpretation during an event that directly disrupts behavior.
Methods
Pre-pandemic data on workers ages 18 to 69 in the 2019 National Health Interview Survey are reweighted to match the distributions of demographic characteristics of Duke University employees surveyed nine months after the pandemic. This latter population had a low risk of infection or economic insecurity. The prevalence, severity, and scores of each of the nine symptoms are compared overall and by age group.
Results
Elevated psychological distress is mainly due to the increased prevalence of particular symptoms .
The prevalence of problems concentrating increased six-fold from 9.6% to 72.5%.
Other symptoms increased by more than a third; feeling anxious, having little interest, feeling depressed, having trouble sleeping, and being irritable, while some symptoms increased by only 10% or less.
Severity also increased, but the magnitudes are small relative to changes in prevalence. The escalation in prevalence and severity is greater for younger people.
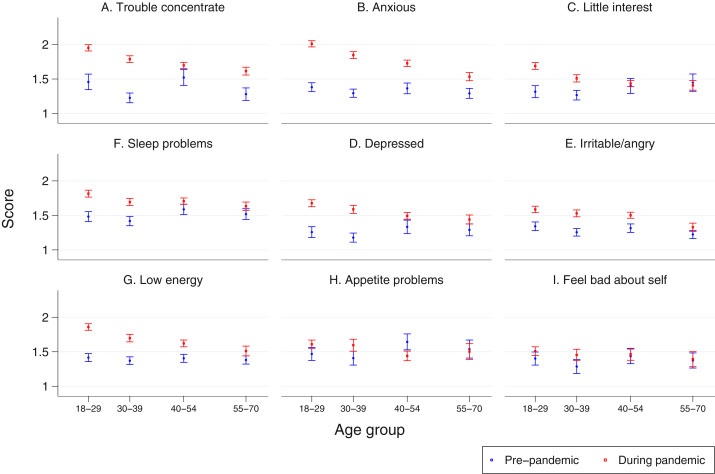
Average scores if a problem is reported, by item and age group
Interpretation
Some of the least prevalent pre-pandemic symptoms became the most frequent during the pandemic, affecting the interpretation of validated pre-pandemic indices.
Clinical and policy interventions should focus on the specific symptoms that increased, including problems concentrating and anxiety.
Discussion
Studies have documented elevated rates of psychological distress early in the COVID-19 pandemic; This distress persisted at least nine months after the pandemic and affected populations with very low risk of infection or economic insecurity.
We document increases in depression and anxiety symptoms that are driven primarily by extremely large increases in the fractions of the population reporting each symptom and these increases vary substantially across symptoms.
Two symptoms stand out: difficulty concentrating and anxiety.
About three-quarters of the study population report each symptom nine months into the pandemic. Additionally, the age gradient of these symptoms is more pronounced; About 5 in 6 of people in the youngest age group (18-29 years) report each symptom nine months into the pandemic.
Large increases in the prevalence of these symptoms are accompanied by substantial increases in severity , particularly for young people, for whom severity increases by approximately 40%.
There are also large increases in the prevalence of having low interest, trouble sleeping, feeling depressed, and feeling irritable or angry, with more than half of respondents reporting these symptoms nine months into the pandemic. Differences in age gradients are less clear for these symptoms. Although the increase in the severity of these symptoms attenuates in relation to the increase in prevalence, severity tends to increase more among younger people.
Taken together, these results raise questions about the comparison and interpretation of indices measured before and during the pandemic. The indices are an average of specific scores for an item, so the weight of each item is the product of the prevalence and severity of that item. As the prevalence distribution has changed dramatically during COVID-19, the weight of each item in an index has also changed.
As an example, using the 7 PHQ-9 items reported here, problems concentrating contribute 7% to the pre-pandemic total score of 1.9, but 22% to the total score of 5.9 during the pandemic. Appetite problems contribute 11% to the pre-pandemic and 6% to the pandemic.
While the psychometric properties of indices validated before the pandemic have not been established for use during the pandemic, it is clear that individual symptoms have been negatively affected. It is critical to understand how specific elements have changed in prevalence and severity; Interventions targeting the highest aspects of psychological distress during the pandemic are likely to have the greatest impact on population health and well-being now and possibly in the future.
In particular, assessment of specific symptoms is critical because the literature suggests that some symptoms are likely to have longer-term deleterious consequences beyond physical and psychological health. For example, difficulty concentrating has been linked to reduced productivity at home, school, and in the labor market.
Several studies using rigorous randomized controlled trials in low-income settings have established that the cognitive load arising from difficulty concentrating results in choices that are less than ideal, leading to reduced levels of health and well-being for individuals and your families. Extremely high rates of difficulty concentrating during the pandemic have likely affected these people’s productivity.
Our results indicate that longer-term impacts are likely to be greater for younger cohorts who are in the process of establishing their career trajectories. While studies have documented associations between productivity and anxiety, poor sleep, and depression, the underlying causal pathways are not well understood. To the extent that elevated rates of these symptoms further contribute to reduced productivity, broadly defined, the epidemic of psychological distress will have lasting effects on population well-being.
Furthermore, these lasting indirect effects are likely to be greater for younger adults, who were at very low risk for the direct health effects of hospitalization or death from COVID-19. Interventions targeting specific symptoms and the most affected population subgroups have the potential to be effective in mitigating the impacts of COVID on psychological distress and its sequelae.
Added value of this study
This study provides evidence from matched cohorts of individuals before and during the COVID-19 pandemic. We disaggregate commonly used indices and show that increases in scores are primarily due to increased prevalence, rather than increased severity. However, among young adults, increases in both prevalence and severity are large and potentially clinically relevant.
Furthermore, we found that the increases are concentrated among specific symptoms and are not evenly distributed across the entire depressive syndrome.
In particular, problems concentrating and feelings of anxiety have increased the most. Many of the least prevalent pre-pandemic symptoms have become the most prevalent.
Implications of all available evidence
The long persistence of adverse mental health during the COVID-19 pandemic, and the prevalence in populations with minimal exposure to infection or economic insecurity, suggest that mental health will continue to be a challenge as the pandemic subsides, particularly among young people. .
This work has further implications for future pandemics and public health emergencies, regarding the specific symptoms that may be most affected. Mental health interventions should consider the specific symptoms that have been most affected, and research results from aggregate indices should be interpreted considering changes in the relative weights of their component symptoms.
Conclusions While the burden of COVID-19 mortality has fallen most heavily on older adults, the burden of psychological distress has affected people of all ages, including those at low risk of infection. The increases are not evenly distributed across all symptoms , but rather are concentrated in a subset of domains, with increases in difficulty concentrating and feelings of anxiety being particularly concerning. Indices based on clinically validated psychometric assessors should be interpreted with this in mind; observed increases in depression and anxiety symptoms during the pandemic have been driven primarily by a sharp increase in the fraction reporting symptoms: more than 5 in 6 people reported problems concentrating and feeling anxious. This epidemic of psychological distress has the potential to have persistent and far-reaching impacts on the health and well-being of the population, broadly speaking, with younger adults being at greatest risk of harmful impacts reaching their future. Interventions targeting specific symptoms can be of great value, especially for younger populations. |
Funding : Trinity College of Arts & Sciences and the Social Sciences Research Institute at Duke University.
















